ACQUIRE CUSTOMERS ON AUTO-PILOT
The Reviews & Messaging Platform For Local Business

Online Reviews
Improve your ratings and build your reputation to win more business.

Messaging
Reach your customers wherever they are.

Payments
Fast, easy, secure payments.
All the tools you need to grow in one place.

Online Reviews
Automate your online reviews with a few simple clicks & respond to reviews in 1 place

Messaging
Manage your messages with a single inbox for text, Facebook messages, Google messages, and more.

Webchat
Convert more website visitors into leads & sales conversations with Webchat.

Payments
Easy text 2 pay client invoicing. Simplify your client invoicing & get paid faster.

Missed Call Text Back
When you're away, have HandiFlow follow up via text so you never lose another customer

CRM
Grow your audience & know where
new leads are coming from
Online Reviews
Automate Your Online Reviews
Improve your ratings, build your reputation, and get found online by sending review requests via text to recent customers, responding to and interacting with reviewers, and managing it all from a single inbox.
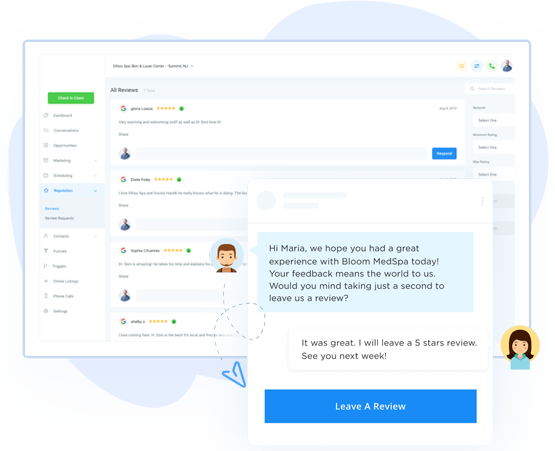

Every Conversation In One Place
Communicate Efficiently With Customers and Leads
Reach your customers wherever they are with text messaging. Request reviews, connect with website visitors, collect payments, respond to Facebook & Google Messages, and market to customers and leads all from your app.
Get Paid Faster Than Ever
Collecting payments isn’t anyone’s favorite job. Make paying as quick and convenient as possible for your customers with a secure payment link delivered right to their phone.


Grow Your Audience
Grow your audience & know where new leads are coming from with HandiFlow's easy-to-use CRM. Easily import existing leads to make client communication a cinch!
Easily Integrates With Leading Apps






Book a Demo
Explore a better way to grow
92 99 62 28
92 99 62 28
Copyright HandiFlow 2022 -- All Rights Reserved
We’re on a mission to build a better future where technology creates good jobs for everyone.
